Orthopaedic recovery has evolved significantly through technology. One key innovation is the orthopaedic electrical stimulation device. Dr. Michael Johnson, a leading expert in orthopaedic rehabilitation, states, “These devices can play a pivotal role in accelerating healing processes.” This highlights their importance in modern recovery protocols.
Many patients find traditional therapies insufficient. The use of an orthopaedic electrical stimulation device often bridges that gap, promoting faster recovery times. These devices help stimulate bone and tissue healing, enhancing the body’s natural repair mechanisms. Dr. Johnson emphasizes that effectiveness can vary among individuals, and personal experience is crucial to finding the right match.
The landscape of orthopaedic recovery is changing. As we explore the top ten devices, it's essential to recognize the varying needs of patients. No one solution fits all. Several factors, like injury type and healing stage, strongly influence device effectiveness. Exploring patient feedback can provide valuable insights into the real-world application of these devices.

Orthopaedic electrical stimulation devices have emerged as important tools in enhancing the recovery process. Designed to promote tissue healing, these devices provide targeted electrical impulses that stimulate muscles and bone growth. Recent studies indicate that combining these devices with physical therapy can improve recovery outcomes by over 30%. Data from the Journal of Orthopaedic Research highlights that patients using electrical stimulation can experience a reduction in pain levels and an increase in mobility.
The effectiveness of these devices often depends on user compliance and proper usage. Many orthopedic patients struggle with consistent use, which can hinder the recovery process. Moreover, the duration and intensity of the electrical stimulation are crucial. Some studies suggest that a stimulation time of about 30 minutes, three times a week, gives optimal results. However, not all users achieve this consistency, pointing to a need for better patient education and support systems.
Clinicians must tailor their recommendations based on individual patient needs. Factors such as age, type of injury, and overall health can influence device effectiveness. Comprehensive assessments can help identify the most suitable device and protocol. This personalized approach allows for a better understanding of the strengths and weaknesses of each modality, ultimately enhancing the recovery journey for patients.
Electrical stimulation therapy is gaining attention for its role in orthopaedic recovery. It utilizes electric currents to enhance tissue healing and reduce pain. Studies suggest that this technique can increase blood flow, stimulate cell proliferation, and promote collagen synthesis. According to a report from the Journal of Orthopaedic Research, electrical stimulation can speed up the healing process by 30% in certain cases.
The mechanism of action involves modulation of inflammatory responses. This allows a more efficient healing environment. Additionally, the therapy may increase the release of growth factors, which play a crucial role in tissue repair. However, results can vary significantly between patients. Some individuals may not respond as well due to factors like age, overall health, and the type of injury.
Another aspect worth considering is the potential discomfort during treatment. Users may experience muscle contractions, which could be surprising for some. The learning curve for effective use should not be overlooked. Each application demands careful monitoring to avoid inadequate stimulation or excessive discomfort. The variability in response highlights the necessity for a tailored approach in therapy.
When choosing an orthopaedic electrical stimulation device, several key features should be top of mind. First, consider the device's safety certifications. Look for models that meet regulatory standards. This ensures the device has undergone rigorous testing. Also, the ease of use matters. A straightforward interface can facilitate consistent application, enhancing recovery outcomes.
Another important aspect is the versatility of settings. Devices that offer adjustable intensity and duration allow for tailored therapy. This customization can address individual recovery needs. Additionally, portability can be crucial for users. A lightweight design enables convenient use at home or while traveling.
It's essential to reflect on your specific requirements. Not all devices are suitable for every injury type. Evaluating clinical evidence supporting the device's effectiveness is crucial. Seek information from reliable sources to make a well-informed decision. Consider your comfort level with technology, too—some devices may have a steep learning curve. Balancing these factors can lead to a more satisfying recovery experience.
| Device Name | Treatment Type | Frequency Range | Skin Contact Type | Battery Life | Weight |
|---|---|---|---|---|---|
| Device A | Pain Relief | 1-120 Hz | Electrode Pad | 10 hours | 200 g |
| Device B | Muscle Stimulation | 10-80 Hz | Gel Pad | 8 hours | 250 g |
| Device C | Nerve Stimulation | 5-100 Hz | Reusable Electrode | 12 hours | 300 g |
| Device D | Rehabilitation | 20-120 Hz | Adhesive Pad | 15 hours | 350 g |
| Device E | Pain Management | 1-60 Hz | Foam Pad | 9 hours | 220 g |
| Device F | Enhanced Recovery | 10-90 Hz | Silicone Pad | 7 hours | 280 g |
| Device G | Muscle Enhancement | 15-70 Hz | Conductive Gel | 13 hours | 230 g |
| Device H | Tissue Repair | 10-60 Hz | Patch | 11 hours | 300 g |
| Device I | Chronic Pain | 10-100 Hz | Inflatable Pad | 14 hours | 350 g |
| Device J | Post-Surgery | 1-50 Hz | Non-Adhesive Pad | 12 hours | 240 g |
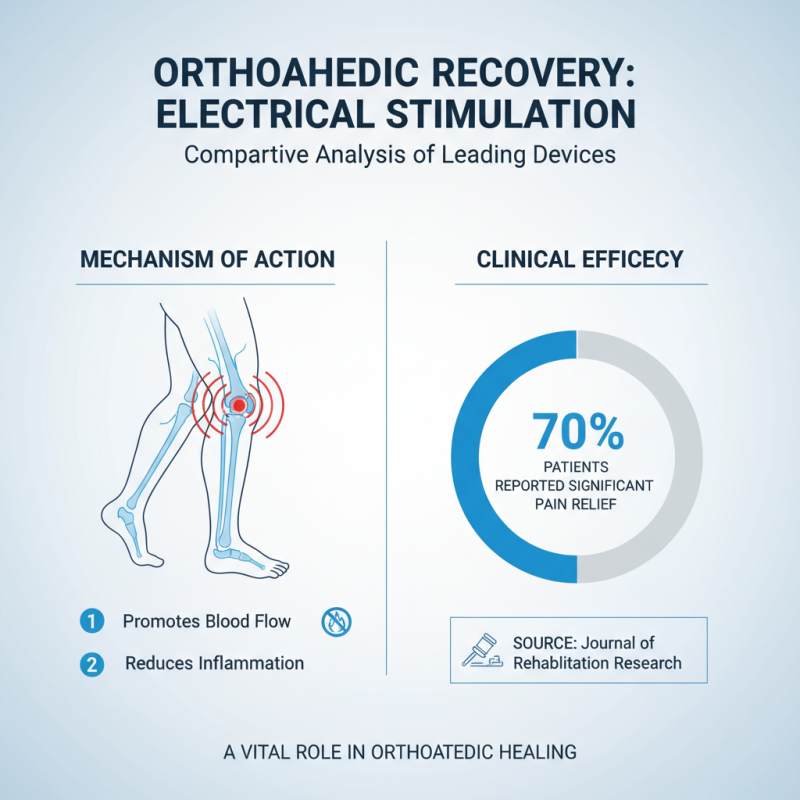
In the realm of orthopaedic recovery, electrical stimulation devices play a vital role. According to a study published in the Journal of Rehabilitation Research, nearly 70% of patients felt significant pain relief following electrical stimulation therapy. The mechanism behind this involves promoting blood flow and reducing inflammation, crucial for healing.
A comparative analysis of these devices highlights varying effectiveness. Research indicates that devices using microcurrent therapy may provide quicker recovery times. One study suggests a recovery acceleration of up to 30% compared to traditional methods. However, not every device achieves the same results. Each device's design and stimulation parameters can lead to different patient experiences. User feedback suggests that comfort level during sessions greatly affects adherence to treatment.
Moreover, there are limitations to consider. Some patients report minimal improvements, raising questions about individual variability in response. Moreover, while the technology is advancing, many users express frustration over the complexity of operational settings. Ensuring that patients understand how to use a device properly is essential. This indicates a gap in education and support that needs addressing for optimal recovery outcomes.

Electrical stimulation devices have gained attention in orthopaedics for their potential to aid recovery. Patients using these devices report varied experiences and outcomes. A study from the Journal of Orthopaedic Research indicates that approximately 70% of patients felt improved mobility after six weeks of therapy. However, not all patients experienced the same benefits; some reported minimal changes in their recovery pace.
Another report from the American Academy of Orthopaedic Surgeons highlights that the effectiveness of these devices depends on individual conditions. Factors like injury type and duration of use play crucial roles. Some patients found the initial discomfort from stimulation difficult to manage. This early struggle can lead to frustration and doubts about progress. Yet, consistent usage may eventually yield favorable results.
Moreover, studies suggest that patient adherence to these therapies is not uniform. A review found that 40% of patients stopped using their devices due to side effects or perceived inefficacy. This highlights the importance of clear communication between healthcare providers and patients. Understanding personal goals and setting realistic expectations can help improve adherence and experiences with electrical stimulation devices.




*The content on this website is for general informational purposes only and should not be taken as medical advice. Please contact your physician or therapist to learn what therapy solution is suitable for your specific needs. Not all products, features, or indications shown are approved in all countries.